Introduction
The Pitt — Episode 4, Stone's collapse:
"Tracheal deviation to the right. 14-gauge angiocath now." — Dr. Robby
[Audible hissing of escaping air]
"Sats coming up. Pressure returning." — Nurse
In seconds, a 14-gauge needle inserted into Stone's chest in The Pitt reverses an imminent cardiovascular collapse. There is no procedure faster, simpler, and more dramatically effective in emergency medicine — and no procedure where a single minute's delay can cost a life.
Needle decompression for tension pneumothorax is one of the life-saving procedures that every emergency physician, paramedic, and — in many jurisdictions — any trained healthcare provider must be able to perform. It is a recognition-and-execution procedure, not an imaging-diagnosis one.
What Is Needle Decompression?
The emergency decompression needle is typically a 14-gauge (14G) over-the-needle IV catheter (angiocath) with a minimum length of 3.25 to 8cm — depending on insertion site and patient habitus. The needle pierces the chest wall into the pleural space, allowing the pressure-accumulated air to escape immediately, relieving compression of the heart and great vessels.
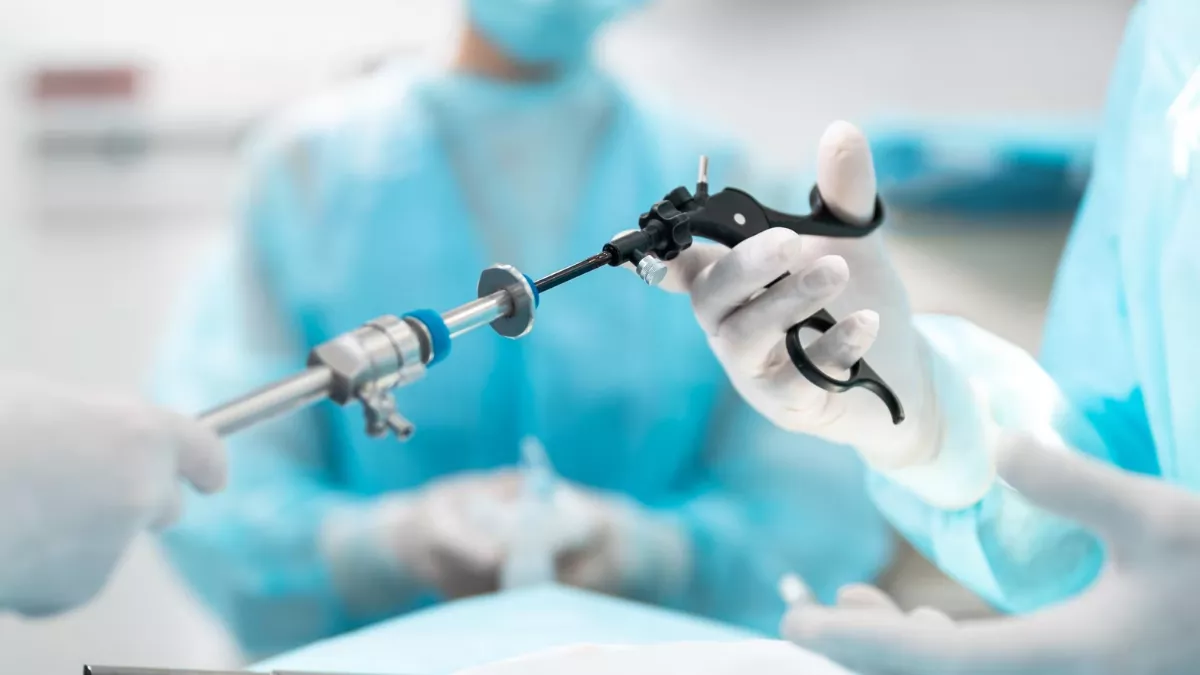
The 14G caliber is not arbitrary — it is the smallest bore that provides sufficient airflow for rapid decompression while maintaining enough rigidity to penetrate the chest wall without bending. Larger calibers (10G-12G) exist in specialized trauma kits, but the conventional 14G IV catheter is the most available and most widely used in practice.
Indications: Clinical Diagnosis, Not Radiological
Needle decompression is indicated for tension pneumothorax — a clinical recognition emergency. Chest X-ray, POCUS, or any imaging study is never awaited before acting. Clinical criteria are:
- Progressive hypoxia refractory to supplemental O2
- Sudden hypotension with systolic below 90mmHg
- Absent or markedly reduced unilateral breath sounds
- Contralateral tracheal deviation — late sign, identified by Dr. Robby in the episode
- Jugular venous distension — may be absent in hypovolemic patients
- Risk context: chest trauma, positive pressure ventilation, recent central venous access
In mechanically ventilated or BiPAP patients, the earliest sign is usually a sudden increase in peak airway pressure with simultaneous saturation drop and hypotension.
Insertion Sites
Two sites are accepted by international guidelines (ATLS, PHTLS, TECC):
2nd Intercostal Space, Midclavicular Line (classic site)
- Location: palpate clavicle → 2nd rib → space above 3rd rib = 2nd ICS
- Reference: Angle of Louis (manubriosternal junction) is at the level of 2nd ICS
- Advantage: easy anatomical landmark, no patient mobilization needed
- Disadvantage: thick pectoral muscle in athletes and obese patients may prevent short needles from reaching the pleural space
4th or 5th Intercostal Space, Anterior Axillary Line (preferred in obese patients)
- Location: follow anterior axillary line to nipple level
- Advantage: thinner chest wall, higher success rate in patients with thick chest wall
- Recommended by ATLS and TCCC as primary site in adults
At any site: insert over the superior rib border to avoid the neurovascular bundle in the subcostal groove.
Technique
- Identify the site: 2nd ICS midclavicular or 4th/5th ICS anterior axillary line
- Quick antisepsis: alcohol or chlorhexidine — no time delay in extreme emergency
- Perpendicular insertion: 14G angiocath, over the superior rib border, with continuous aspiration
- Confirm position: audible hissing of escaping air — immediate and unequivocal confirmation
- Remove the stylet: keep only the flexible plastic catheter in place
- Observe clinical improvement: SpO2 rising, blood pressure returning, heart rate dropping — as seen in Stone's case
- Do not fix permanently: the decompression catheter is temporary — definitive drainage with pigtail or chest tube must follow immediately
Needle Decompression Failures
Decompression fails in 25 to 40% of cases with a conventional 3.25cm needle in patients with thick chest walls. Failure causes:
- Needle too short: does not reach the pleural space in obese or muscular patients — use 8cm needle or axillary site
- Catheter bending: plastic catheter bends within soft tissues — use reinforced metal catheter when available
- Tissue plug: subcutaneous tissue plug obstructs the tip
- Wrong diagnosis: if there is no hissing and no clinical improvement, consider alternative diagnoses (cardiac tamponade, massive pulmonary embolism)
If needle decompression fails: try a second site (anterior axillary line) or proceed immediately with chest tube without waiting for additional imaging.
Prognosis & Complications
When the tension pneumothorax diagnosis is correct, needle decompression reverses the condition in seconds — as dramatically demonstrated by Stone. Prognosis is excellent when intervention occurs before complete cardiovascular collapse.
Possible complications:
- Lung injury: if needle is inserted with adjacent lung expanded — low risk in tension pneumothorax, where the lung is collapsed
- Intercostal artery injury: insertion over the inferior rib border
- Iatrogenic pneumothorax: if the diagnosis is wrong and the lung is punctured — real risk, but benefit outweighs risk in clinically confirmed tension pneumothorax
- Gas embolism: extremely rare with correct technique
Frequently Asked Questions
Why 14G and not a larger needle?
14G offers the ideal balance between sufficient airflow for rapid decompression and enough rigidity to penetrate the chest wall without bending. Larger calibers (10G-12G) exist in specialized kits but are less available. Smaller gauges (16G-18G) have higher bending risk and insufficient flow. The conventional 14G is the most universally available and validated option.
Which site to choose — midclavicular or anterior axillary?
For normal-habitus patients: either. For obese, muscular, or thick-chested patients (above 3cm): prefer the anterior axillary line (4th/5th ICS), where the chest wall is thinner and success rates are higher. The latest ATLS (10th edition) recommends the anterior axillary line as the primary site for adults.
What to do after needle decompression?
Needle decompression is temporary — the catheter can bend or obstruct. Definitive chest drainage with pigtail catheter or conventional chest tube must be performed as quickly as possible after clinical stabilization. Confirmatory chest X-ray after the procedure.
Can any healthcare provider perform needle decompression?
In many pre-hospital emergency protocols (ATLS, TECC, PHTLS), needle decompression for tension pneumothorax is included in advanced paramedic and military medic competencies. In hospital settings, it is primarily an emergency physician competency, but can be delegated in extreme urgency. Periodic training is essential — this procedure needs to be automatic.
Conclusion
The 14G needle in The Pitt represents one of emergency medicine's most powerful maneuvers: simple, fast, inexpensive, and capable of reversing imminent cardiovascular collapse in seconds. What makes this gesture possible is not sophisticated equipment — it is immediate clinical recognition and the willingness to act without waiting for imaging confirmation.
See also: Pigtail Catheter, Tension Pneumothorax from BiPAP, and Pneumothorax from Pulmonary Contusion.
This content is for educational purposes only and does not substitute professional medical evaluation, diagnosis, or treatment. In case of emergency, call 911 immediately.